Warren’s Story
“The more research you do, the more invested you get, and it becomes more and more meaningful.”
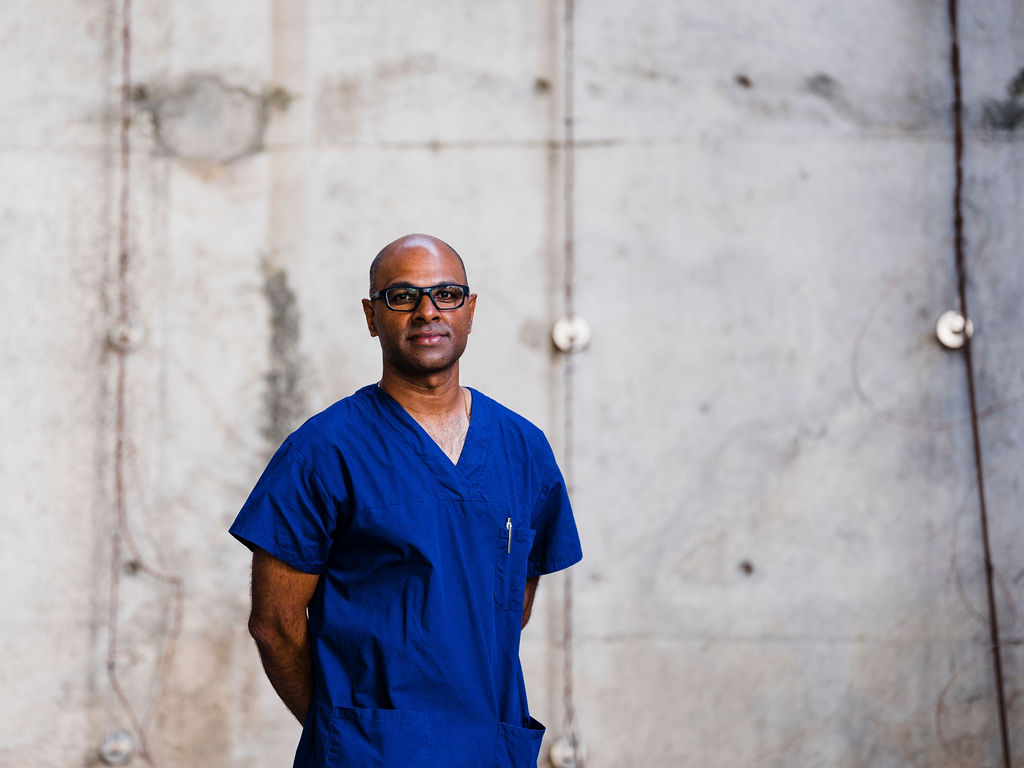
“The more research you do, the more invested you get, and it becomes more and more meaningful.”

The cardiac anaesthetist performs a vital and highly specialist role during heart surgery, arresting and monitoring the organ while surgeons operate.
“We interact a lot with the surgeon. We are relaying lot of information to them, we use echo to look at the heart to see how it’s going while they’re operating on it to help guide them with their work,” he explains.
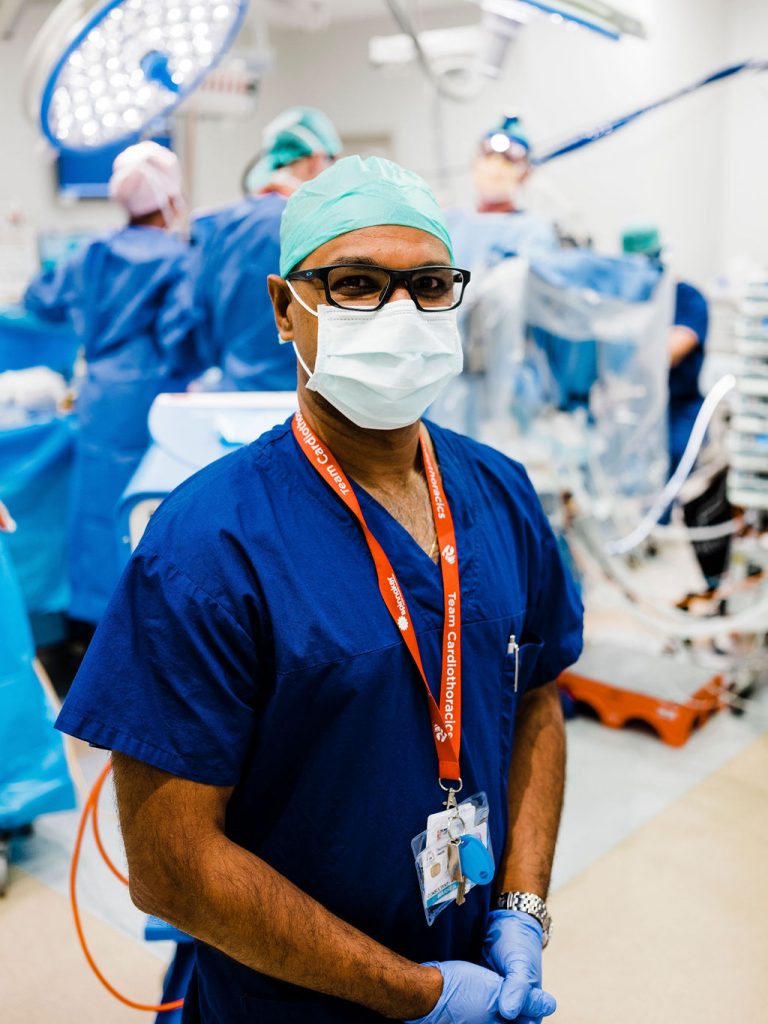
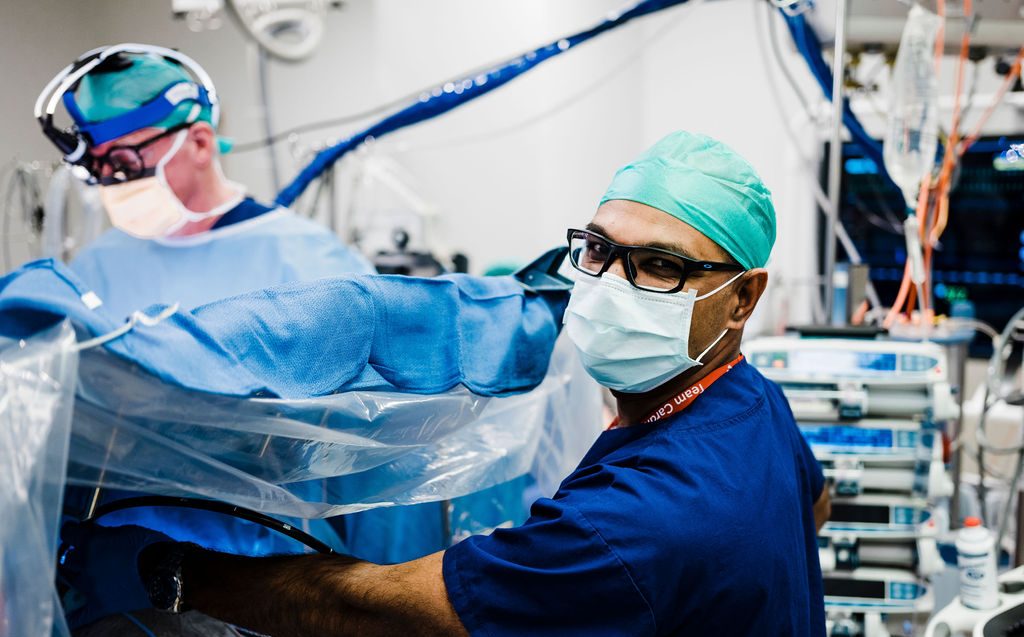
It’s during the delicate restarting stage that the heart needs a little help. His measured tone, generous nature and meticulous attention to detail mean those vulnerable hearts are in very good hands.
“When the heart’s fixed we have to start it up again and wean it off the machine … so you have to drive it with drugs to make sure its pumping hard enough. People think we just put people to sleep and wake them up but that’s the smallest part of the job.”
Warren waxes lyrical about this most mythical and magical of organs.
Warren, you see, loves hearts.
“It’s just cool seeing a heart beating,” he says with a childlike enthusiasm. “We turn it on and off — we arrest the heart and then restart it. Every time you see it, it’s an amazing thing. All organs do their own thing but this is doing its thing visibly. A liver sits there and you can’t really see it doing anything but a heart, you can see it working and you can see when it’s not working.”
It’s when someone’s heart isn’t working well that they might meet Warren. Indeed, as well as being a key theatre team member in heart surgery, he’ll likely play a role in most of the 15-or-so heart transplants performed each year at Fiona Stanley Hospital.
But as busy as he is, Warren would love to see the hospital do more. Disheartened by the number of donor organs that have to be discarded because they’re considered unviable, Warren is determined to find ways to properly assess so-called “marginal” hearts so they can be implanted and save lives.
Though his work tackles issues that affect hospitals wordwide, it is particularly important in farflung Perth: while we can send organs to the east coast, headwinds that can add an hour to the flight time mean we cannot receive theirs. “Kind of like the GST,” Warren says with a laugh.
Warren’s important research touches on three key areas: trying to keep fragile, energy-hungry hearts alive longer outside the body, finding fast, effective and cheap ways of testing donor hearts and discovering simpler and more affordable ways of caring for “dead” hearts.
Traditional donors, Warren explains, are brain dead: their heart is still beating but they will never regain consciousness. But there is another pool of donors whose hearts have stopped.
“A small but significant number of people that die in that way that have agreed to donate their organs that don’t fit the standard donation method. That’s called donation after circulatory death. Until now we haven’t been able to use those hearts,” he says.
In hospitals such as St Vincent’s in Sydney, a wildly expensive “heart in a box” machine keeps the heart alive while fairly “crude” methods involving a fair bit of guess work are used to assess the heart’s viability.
Warren’s dream is that the gifts so graciously given by donors will be used to save a life rather than be discarded.
The former Aquinas student is driven by a desire to “do better” for patients.
“The more research you do, the more invested you get and it becomes more and more meaningful,” he says.
“I’ve seen organs go to waste and … when we use them I think we could handle them and manage them a lot better than we do. And then the patient would benefit hugely. We should be giving them the best organ we can, in the best condition. And I think we can do that if we try.”
Donate today to support research